Alopecia Areata
Background
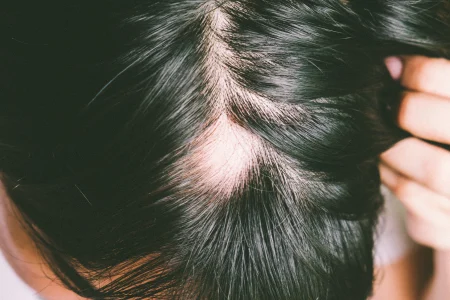
Alopecia areata is an autoimmune condition that causes the body to attack the hair follicles, resulting in hair loss. Typically, this condition is characterized by round patches of non-scarring hair loss; and occasionally, nails changes.
It is estimated that the lifetime risk of alopecia areata is approximately 2%. According to the data, 25 to 36 years of age seems to be the average age of onset.
Etiology
It has been hypothesized that the loss of immunity associated with anagen hair follicles plays a key role in the pathogenesis of this disease. Also, genetic factors are involved in disease susceptibility and severity.
Comorbidities
Alopecia areata was found to be associated with several comorbidities, including depression, anxiety, and other autoimmune diseases, such as thyroid disease, lupus erythematosus, vitiligo, psoriasis, rheumatoid arthritis, and inflammatory bowel disease.
Clinical features
Alopecia areata may present in different patterns. Patchy alopecia areata is the most common pattern; it is characterized by well-circumscribed round/oval patches of hair loss with normal skin appearing. Other less common patterns include, alopecia totalis which presents as complete loss of scalp hair, and alopecia universalis which presents as complete loss of body hair.
The scalp is most commonly affected by this condition, but any other area that bears hair can also be affected. The involvement of nails is generally indicative of a more severe type of hair loss. Usually, this condition manifests itself within a short period of time and may progress to the point of hair loss.
Diagnosis
Typically, alopecia areata is diagnosed based on the clinical features of the condition. Additionally, there are several helpful tools that can help support the diagnosis, including dermatoscopes, hair pull tests, and skin biopsy. Dermoscopic findings of active disease include exclamation point hairs, broken hairs, yellow dots, and black dots.
Management
Alopecia areata has an unpredictable course and may improve on its own. There is a wide range of treatments that is available for the management of alopecia with varying degrees of success. Generally intralesional and topical corticosteroids are considered first-line treatment for most patients.
For mild cases, options include Intralesional corticosteroid injections, topical treatments with corticosteroids or minoxidil. For more advanced cases, topical immunotherapy is used. Systemic therapies are reserved for severe or refractory diseases, including systemic glucocorticoids and immunosuppressants such as cyclosporine and methotrexate. The FDA has recently approved Baricitinib, which is a JAK inhibitor with promising outcomes for alopecia treatment.
Written by
Ghida Altammami, medical student
Revised by
Maee Barakeh, medical student
References
DermNet
National Library of Medicine
Bolognia textbook of dermatology