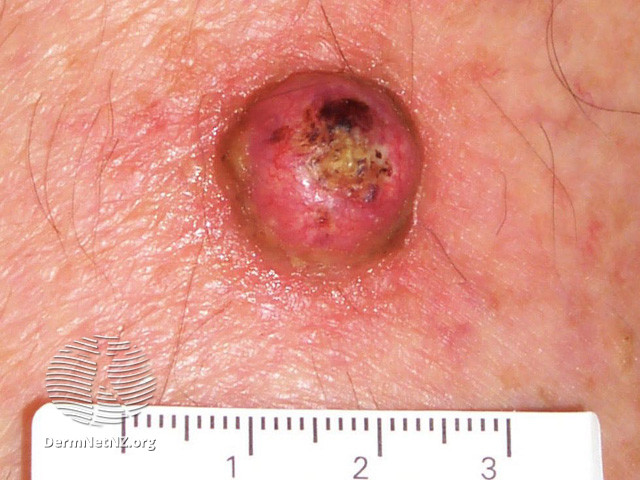
Keratoacanthoma
Keratoacanthoma (KA) is a commonly encountered skin tumor that presents a captivating clinical challenge due to its rapid growth and locally destructive nature. While some cases of KA may regress spontaneously, they often leave behind visible scarring. However, the clinical presentation of KA can closely resemble well-differentiated squamous cell carcinoma (SCC), leading to unpredictability in its course.
Pathophysiology:
The precise pathophysiological mechanisms underlying keratoacanthoma are not fully understood. However, it is widely believed to arise from the hair follicles or the sebaceous glands. Several hypotheses have been proposed, including the role of ultraviolet radiation, genetic factors, viral infections, and immune dysregulation in the development of keratoacanthoma.
Clinical Features:
Keratoacanthoma typically presents as a rapidly growing dome-shaped nodule with a central crater filled with keratin debris. It commonly occurs on sun-exposed areas of the body, such as the face, scalp, ears, and dorsum of the hands. Initially, the lesion may resemble a pimple or a wart, but it rapidly enlarges over a period of weeks to months. The growth phase is followed by a stabilization phase, during which the lesion may persist for several months before spontaneously regressing.
Diagnosis:
The diagnosis of keratoacanthoma is primarily based on clinical examination and histopathological evaluation. A thorough physical examination, including a dermatoscopic assessment, can aid in distinguishing keratoacanthoma from other skin lesions. Dermoscopy often reveals a central plug, keratin-filled crater, and peripheral keratotic rim. To confirm the diagnosis, a skin biopsy is performed, and the specimen is sent for histopathological analysis. Microscopically, keratoacanthoma is characterized by a well-demarcated cup-shaped lesion with a central keratin-filled crater, hyperkeratosis, and proliferation of keratinocytes.
Management:
The management of keratoacanthoma depends on various factors, including the size, location, and individual patient characteristics. Several treatment options are available, and the choice of therapy should be tailored to the specific case. Here are some commonly employed management strategies:
1. Observation: In some cases, keratoacanthomas may undergo spontaneous regression without any intervention. Close observation with regular follow-up visits may be appropriate for small, asymptomatic lesions in low-risk areas.
2. Surgical Excision: Surgical excision is a commonly employed treatment modality for keratoacanthoma. It involves complete removal of the lesion with a margin of healthy tissue to reduce the risk of recurrence. This approach is particularly suitable for larger or symptomatic tumors.
3. Mohs Micrographic Surgery: Mohs surgery is a specialized technique that ensures the highest cure rate while preserving as much healthy tissue as possible. It is often recommended for lesions in cosmetically sensitive areas or those with aggressive features.
4. Topical Therapies: In select cases, topical treatments such as imiquimod cream or 5-fluorouracil may be employed. These medications stimulate the immune system or inhibit cell proliferation, leading to tumor regression.
5. Cryotherapy: Cryotherapy involves freezing the lesion with liquid nitrogen. It is commonly utilized for smaller keratoacanthomas and can be performed in an outpatient setting.
Written by:
Deemah AlHuraish, medical student.
Revised by:
Maee Barakeh, medical student.
References:
DermNet
NCBI
AOCD