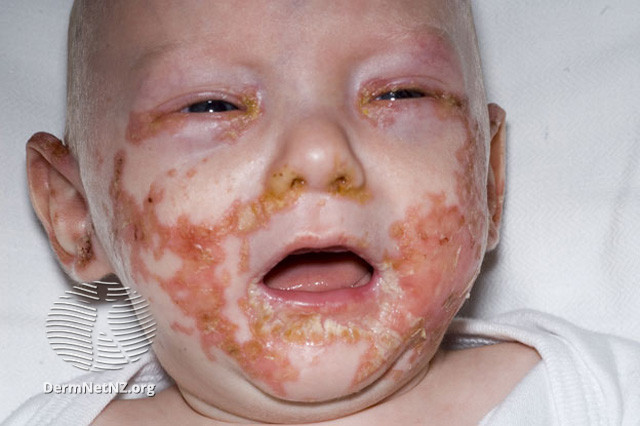
Acrodermatitis Enteropathica
Acrodermatitis enteropathica (AE) is a rare genetic disorder characterized by impaired zinc absorption, resulting in zinc deficiency. This condition affects the skin, gastrointestinal system, and immune system.
Pathophysiology:
Acrodermatitis enteropathica is primarily caused by mutations in the SLC39A4 gene, which encodes for the zinc transporter protein known as ZIP4. This protein plays a crucial role in facilitating the absorption of dietary zinc from the intestines into the bloodstream. Mutations in the SLC39A4 gene lead to impaired zinc uptake, resulting in zinc deficiency despite an adequate zinc intake.
Clinical Features:
Clinical manifestations usually appear within 1 to 2 weeks after weaning or at 4 to 10 weeks of age if bottle-fed.
Acrodermatitis enteropathica is characterized by a classic triad of symptoms, including periorificial dermatitis, diarrhea, and alopecia.
- Periorificial Dermatitis:
The rash in acrodermatitis enteropathica typically presents with a distinct distribution. The periorificial rash is commonly observed in a horse-shoe or U-shaped pattern, involving the areas around the mouth and eyes, while sparing the lips. There is usually a sharp demarcation between the affected area and normal skin, creating a noticeable contrast. The rash may manifest as eczematous or psoriasiform plaques that can progress to include vesicles, bullae, pustules, erosions, or hyperkeratotic areas.
- Diarrhea:
Diarrhea is a common symptom in acrodermatitis enteropathica and is often chronic in nature.
- Alopecia:
Another characteristic feature of acrodermatitis enteropathica is diffuse hair loss, which affects the scalp, eyebrows, and eyelashes. The hair loss may be patchy or diffuse and is attributed to the disruption of hair follicle development and maintenance due to zinc deficiency.
In addition to the triad, acrodermatitis enteropathica can present with various additional cutaneous manifestations. These include glossitis, characterized by a red and glossy tongue, along with mouth ulcers and angular cheilitis. Symmetrical peri-anal excoriations and a rash on the buttocks can also occur. Zinc deficiency can impair wound healing, resulting in delayed healing of cuts and abrasions. Nail changes, such as softness, ridging, abnormal growth, and inflammation of the nail fold (paronychia), may also be observed.
While the noncutaneous symptoms of acrodermatitis enteropathica include blepharo-conjunctivitis, sensitivity to light, loss of appetite, irritability, depressed mood, growth failure in untreated children, hypogeusia, and hypogonadism in male adolescents and young adults.
Diagnosis:
The diagnosis of acrodermatitis enteropathica is primarily based on clinical features and confirmed by laboratory tests. A thorough physical examination, including a detailed evaluation of the skin and mucous membranes, can provide valuable diagnostic clues. Additionally, a detailed medical history, including feeding patterns and response to zinc supplementation, is essential.
Laboratory investigations play a crucial role in confirming the diagnosis. Blood tests can reveal low serum zinc levels, which is a strong indicator of zinc deficiency.
Management:
The management of acrodermatitis enteropathica involves lifelong zinc supplementation to correct the underlying deficiency. Zinc supplementation can be administered orally or, in severe cases, intravenously. The dosage and duration of zinc supplementation are individualized based on the severity of symptoms and response to treatment.
In addition to zinc supplementation, it is essential to address any associated complications. This may include the treatment of skin infections, nutritional support to correct deficiencies of other nutrients, and management of gastrointestinal symptoms such as diarrhea and vomiting.
In conclusion, acrodermatitis enteropathica is a rare genetic disorder characterized by impaired zinc absorption and resulting in zinc deficiency. It presents with a triad of symptoms involving the skin, gastrointestinal system, and immune system. Early diagnosis and lifelong zinc supplementation are crucial in the management of this condition to prevent complications and improve overall health outcomes for affected individuals.
Written by:
Deemah AlHuraish, Medical Student.
Revised by:
Maee Barakeh, Medical Student.
References:
DermNet.
NCBI.
Bolognia Textbook of Dermatology.