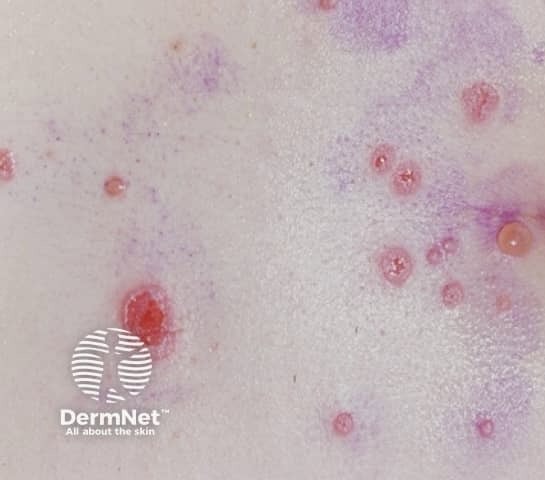
Pemphigus Vulgaris
Definition:
Pemphigus vulgaris is a rare autoimmune disorder characterized by painful blisters and erosions on the skin and mucous membranes, typically seen in the oral cavity. Pemphigus vulgaris is responsible for 70% of all cases of pemphigus globally.
Epidemiology:
Pemphigus vulgaris can occur in individuals of any race, age, or gender. The condition often manifests itself in individuals aged 30 to 60 and is more prevalent among individuals of Jewish and Indian descent compared to other ethnic groups, perhaps due to hereditary factors.
Drug-induced pemphigus is a recognized condition that is mostly caused by penicillamine, angiotensin-converting enzyme inhibitors, angiotensin receptor blockers, and cephalosporins.
Etiology:
Pemphigus vulgaris is a blistering autoimmune disease.
Keratinocytes are adhered together at distinct adhesive sites known as desmosomes. Pemphigus vulgaris is a condition where autoantibodies of the immunoglobulin type G (IgG) attach to a protein called desmoglein 3 (dsg3). This protein is located in the desmosomes of the keratinocytes, which are in the lower part of the epidermis. The outcome is the keratinocytes undergo separation, leading to their replacement by fluid, resulting in the formation of a blister. Approximately half of the individuals diagnosed with pemphigus vulgaris have anti-dsg1 antibodies.
Clinical features:
The majority of individuals with pemphigus vulgaris initially exhibit lesions on the mucous membranes, specifically in areas such as the mouth and genitals. Blisters often form on the skin within a few weeks or months, however in certain cases, only mucosal lesions may be present as a manifestation of the disease.
Skin lesions manifest as thin-walled flaccid blisters containing transparent fluid that easily rupture resulting in itchy and painful erosions. They primarily occur on the upper chest, back, scalp, and face. Erosions occurring in the skin folds have the potential to progress into vegetative lesions characterized by a granular and crusty appearance, a condition known as pemphigus vegetans.
Characteristics of oral mucosal pemphigus include:
- Oral lesions are seen in 50-70% of individuals.
- Shallow blistering and erosion.
- Widespread engagement inside the oral cavity.
- Painful, slow-healing ulcers.
- Difficulty eating and drinking.
- Spread to the larynx, resulting in hoarseness when talking.
Diagnosis:
A biopsy of a blister is typically necessary to diagnose pemphigus vulgaris. The histological examination usually reveals keratinocytes that are rounded and separated (acantholytic cells) located immediately above the basal layer of the epidermis.
Pemphigus is confirmed by the use of direct immunofluorescence staining on skin biopsy sections taken from areas surrounding the lesions. This staining process helps to identify the presence of immunoglobulin (Ig)G antibodies or complement on the surfaces of keratinocytes.
Treatment:
The main objective of treating pemphigus vulgaris is to reduce the occurrence of blisters, prevent infections, and facilitate the healing process of blisters and erosions. Systemic corticosteroids are the primary method of medical treatment for managing the condition. Typically, this involves administering moderate to high dosages of oral prednisone or prednisolone or using pulsed intravenous methylprednisolone. Corticosteroids do not provide a cure for the disease, but they enhance the patient’s quality of life by decreasing disease activity. Administering the necessary dosages of corticosteroids to manage pemphigus vulgaris and the duration of treatment might lead to significant adverse effects and potential hazards.
The duration of therapy and the corticosteroid dosages required to manage pemphigus vulgaris can have major risks and adverse effects.
Patients with pemphigus vulgaris may require other immunosuppressive drugs for years in order to lower the dosage of steroids. These are typically:
- Azathioprine
- Mycophenolate mofetil
- Cyclophosphamide
- Rituximab.
Topical therapy— refers to the use of medications or treatments that are applied directly to the skin or mucous membranes to treat a specific condition or disease.
Topical treatment for cutaneous pemphigus vulgaris may involve the use of topical corticosteroids and moisturizers.
The management of mucosal pemphigus vulgaris may involve the use of different preparations of a topical corticosteroid, intralesional corticosteroid, topical tacrolimus, or topical ciclosporin.
General management:
Proper wound care is crucial, as it helps facilitate the healing process of blisters and erosions.
- When changing dressings, it is important to wear surgical gloves and follow the aseptic method.
- Analgesics may be necessary, particularly when changing dressings.
- Drain blisters that are still intact, but maintain the blister roof.
- Apply non-adherent dressings (silicone mesh or gauze soaked in petrolatum, for example).
- Patients should limit activities that may damage the skin and mucous membranes while the condition is active. These activities include contact sports and eating food that has the potential to irritate or injure the oral cavity, such as spicy, acidic, hard, and crunchy meals.
Maintaining oral hygiene and practicing adequate dental care are crucial.
Written by:
Mashael Alanazi, Medical student
Revised by:
Naif Alshehri, Medical Intern
Resource:
DermNet