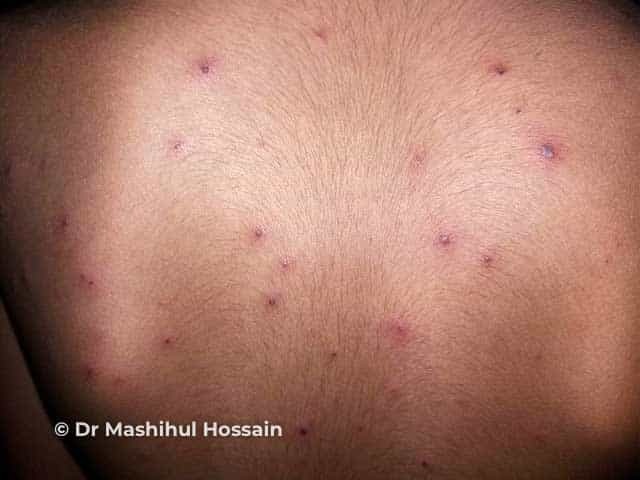
Chickenpox
Introduction and Epidemiology:
Chickenpox is a highly contagious viral infection that causes an acute fever and blistered rash, mainly in children. Varicella virus is the etiologic agent of chickenpox. Varicella zoster virus has a worldwide distribution and 98% of the adult population is seropositive. In the pre-vaccine era, 90% of children <10 years of age developed varicella and ~4 million cases occurred annually in the US, with large outbreaks during the winter and spring. Since the introduction of the varicella vaccine in 1995, the overall incidence of varicella has decreased by ~85%, with evidence of herd immunity.
Pathogenesis:
Airborne droplets are the usual route of transmission of varicella, although direct contact with vesicular fluid is another mode of spread, and the incubation period is 11–20 days. Varicella is extremely contagious, and 80–90% of susceptible household contacts develop a clinically evident infection. The affected individual is infectious from 1–2 days before skin lesions appear until all the vesicles have crusted.
Clinical features:
A prodrome of mild fever, malaise, and myalgia may occur, especially in adults. This is followed by an eruption of pruritic, erythematous macules and papules, which starts on the scalp and face, and then spreads to the trunk and extremities. Lesions rapidly evolve over 12 hours into 1–3 mm clear vesicles surrounded by narrow red halos (“dew drops on a rose petal”). The number of vesicles varies from only a few to several hundred, and there is often involvement of the oral mucosa. Sparing of the distal and lower extremities is common. Older vesicles evolve to form pustules and crusts, with individual lesions healing within 7–10 days. The presence of lesions in all stages of development is a hallmark of varicella. The disease course is usually self-limited and benign in healthy children. Secondary bacterial infection of the skin with subsequent scarring is the most common complication. CNS sequelae are uncommon ( <1 per 1000 cases) and may include encephalitis and acute cerebellar ataxia. Reye syndrome which consists of encephalitis plus fatty liver is now rare due to avoidance of aspirin in children with varicella. Varicella in adolescents and adults is often more severe than in children, with an increased number of skin lesions.
Diagnosis:
A clinical diagnosis can usually be made based upon the history, including previous varicella or vaccine administration, and physical examination. A Tzanck smear, PCR or DFA can assist in quickly confirming the diagnosis.
Treatment:
Varicella in immunocompetent children can be treated symptomatically with antipyretics (e.g. acetaminophen), antihistamines, calamine lotion, and tepid baths. If started within 24–72 hours after the onset of the cutaneous eruption, acyclovir has been shown to decrease the duration and severity of varicella. Oral acyclovir and valacyclovir are FDA-approved for the treatment of varicella in children (2–17 years of age) while acyclovir is approved for adults. These antiviral agents are recommended for varicella in healthy adolescents and adults as well as in children with chronic cutaneous or pulmonary disorders and in those receiving chronic salicylate therapy, inhaled corticosteroids, or intermittent oral corticosteroids. However, routine antiviral therapy is not recommended for otherwise healthy children with varicella due to the self-limited disease course and modest benefits of treatment.
Written by:
Bandar Alharbi, Medical Intern
Revised by:
Naif Alshehri, Medical Intern
Resources:
Bolognia 5th edition
Dermnet
MOH