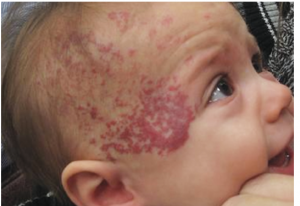
Hemangioma and PHACES Syndrome:
Hemangioma is the most common benign vascular tumor of infancy. It is more common among baby girls than boys (3:1). Low birth-weight, advanced maternal age, multiple pregnancy (twins and triplets), placenta previa and preeclampsia are all risk factors for developing infantile hemangioma. It is believed that the expression of GLUT1 protein in utero is the placental origin for infantile hemangioma.
Most hemangiomas don’t occur at birth but appear within the first two weeks of life, most commonly on the head and neck area. It usually starts off as a red spot resembling a scratch, but instead of fading away, it gradually grows. Most infantile hemangiomas grow very rapidly in the first 3 months, they tend to have a growth arrest by 5 months of age, and recede over the next couple of years. Hemangiomas could be superficial or deep; superficial hemangioma appear bright red, while deep hemangioma appear bluish-purple in color. The majority of hemangiomas are focal, but could occasionally present as segmental or multifocal.
Hemangioma could arise on its own or as a part of PHACES Syndrome, which was first described by Dr. Ilona Freidan in 1996. It is a syndrome that includes infantile haemangiomas and malformation of eyes, heart, arteries and brain. The acronym PHACES stands for: Posterior fossa abnormalities, Hemangioma, Arterial abnormalities, Cardiac abnormalities, Eye and Endocrine abnormalities and Sternal clefts.
Segmental haemangioma is more likely to be associated with PHACES syndrome when compared to focal haemangiomas. Moreover, the specific site of the segment affected by hemangioma can indicate the likely problem associated with it. For example, frontotemporal segments are associated with brain malformations, and mandibular segments are associated with cardiac anomalies and airway hemangiomas.
Infants with hemangiomas larger than 24 cm on the face or scalp should undergo investigations to screen them for PHACES syndrome. Investigations include MRI, MRA, CTA, Eye examinations, ear examinations, audiometric testing, echocardiogram and U/S for blood vessels.
The management of PHACES syndrome is tailored to each child depending on the involved organs. Careful evaluation of major blood vessels in the brain and heart should be undertaken prior to initiating propranolol.
Written by: Rema Aldihan, medical student.
References:
https://www.ccakids.org/assets/syndromebk_hemangiomas.pdf