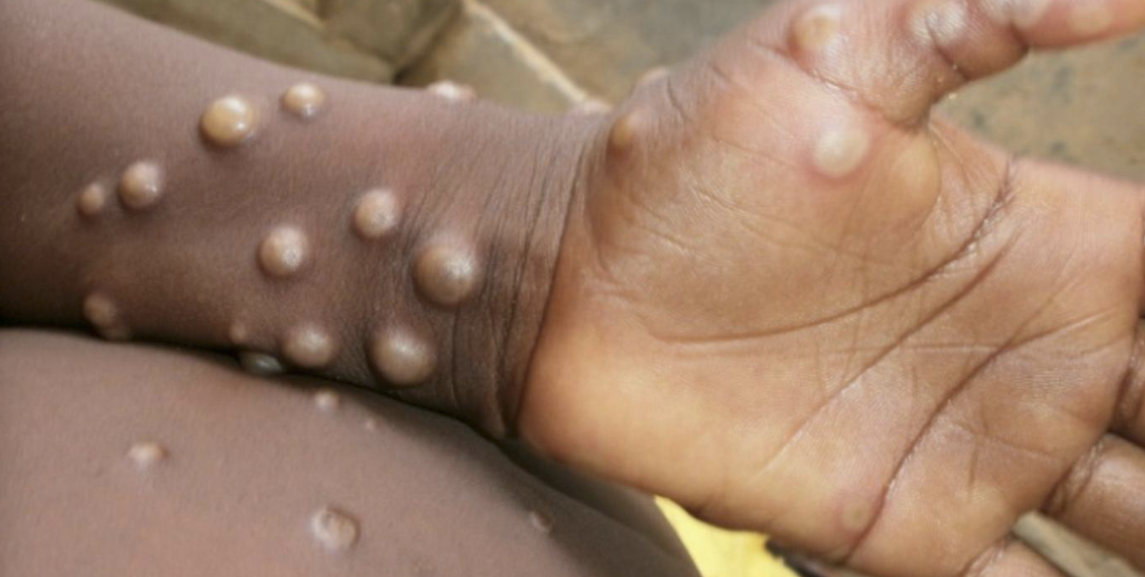
Monkeypox
Monkeypox virus belongs to the orthopoxvirus genus. Orthopoxvirus is a genus of viruses in the family Poxviridae –the same family as cowpox and smallpox. Monkeypox is endemic in several African countries. Since 13 May 2022, several cases of monkeypox have been reported outside the endemic countries. Surprisingly, there hasn’t been any established travel links to endemic areas in those cases. Moreover, the current outbreak of monkeypox is evolving, as the number of cases is changing rapidly.
Transmission:
Monkeypox virus is transmitted from person to person through contact with body fluids or lesion material, contact with fomites, or exposure to respiratory secretions. Fortunately, monkeypox is not easily transmitted.
Diagnosis:
The diagnosis of monkeypox virus requires a 2-step process to be done on the specimen. First is the OPX DNA testing to confirm the presence of orthopox virus –CDC is currently treating all orthopox virus cases as monkeypox until proven otherwise. The second step is a PCR test (only available at CDC) which confirms monkeypox virus.
Clinical features:
Monkeypox initially begins as a flu-like illness with fever and lymphadenopathy –lymphadenopathy is a key clinical feature that helps differentiate monkeypox from smallpox. Then a centrifugal rash erupts; rash starts as macules>papules>vesicles>pustules>scabs. Lesions usually appears simultaneously and evolve together at any part of the body, eg. pustules on the face and vesicles on the arm. Lesions are well circumscribed, deep seated and are occasionally umbilicated. Lesions could be pruritic or painful.
Treatment:
All specimens reported outside of endemic countries, to date, are from the West African clade of monkeypox. This variant is associated with milder illness, therefore, supportive treatment is usually sufficient. Nevertheless, there are 2 CDC-approved therapies to be used in severe cases of monkeypox: tecovirimat and Vaccinia Immune Globulin Intravenous (VIGIV).
Written by: Rema Aldihan, Medical student.
References:
https://www.who.int/emergencies/disease-outbreak-news/item/2022-DON385